Guests
by Siddhartha Mukherjee, November 19, 2010 9:46 AM
 A 46-year-old woman diagnosed with breast cancer had one burning question at the beginning of our meeting: is stress related to cancer? She was in the midst of a gut-wrenching separation from her husband. She was juggling work, finances, responsibilities, child care, and in the midst of all this, had been struck by breast cancer. Had she unleashed her tumor through stress? The quick, if unsatisfying, answer is that we don't know. Five years ago, I would have been less agnostic. Most likely, I would have said: "stress certainly can exacerbate the psychic symptoms that accompany cancer — anxiety, fear, depression, guilt. But to blame cancer on stress is to enter a cycle of blame and victimhood that can be debilitating. Cancer patients often need to summon incredible reservoirs of resilience, and stress can deplete that reservoir in some and activate it in others. And stress, of course, can enable behaviors that are cancer-linked, such as smoking. But the role of stress in directly causing cancer remains speculative. Recently, I've begun to change the way that I think — in part, because of an astonishing experiment performed recently in mice. In this experiment, one group of mice bearing tumors were kept in "stimulating environments" — with other mice and with toys and mazes. The other group was maintained in a "normal" environment, the standard cage in a laboratory (which, while designed to be quite comfortable for mice, does not "stimulate" them). The surprising result is that mice in the stimulated environment developed smaller tumors, and occasionally developed tumors that did not grow as aggressively. When the reasons behind this difference were analyzed, the researchers could track it down to a hormone called leptin, which plays a role in metabolism, growth, fat regulation and — you guessed it — stress. This is a mouse experiment in an artificial laboratory setting. It has been criticized by scientists who claim that prior work has never revealed such an obvious link. And it's impossible to generalize it to humans. But it allows us to begin to address the link between cancer and stress in a more mechanistic, rigorous manner. That is a crucial advance.
|
Guests
by Siddhartha Mukherjee, November 18, 2010 11:01 AM
 Patients often ask me, are we winning or losing the War on Cancer? It is a worthy question, but notoriously difficult to answer. To start with, the very definition of "winning" comes into question. How does one measure victory, or defeat? Take, for instance, a seemingly obvious proposal about the measurement of progress. What if we created a catalog of all major forms of cancer — lung, breast, prostate, colon, and so forth — and measured the fraction of patients who survive five years, or one year, after being diagnosed with each form. Has that fraction changed between 1970, say, and 2010? If only 5% of patients were surviving at 5 years in 1970, and that number is now 20%, can we legitimately use that change as a measure of victory? No — because using survival rate as a guide for progress is inherently sensitive to biases. To understand these biases, imagine identical twins living in neighboring houses — call them Hope and Prudence. Now imagine that a new diagnostic test is introduced that detects early breast cancer. Hope chooses to be screened by the test. Prudence, suspicious of medicine, chooses to forego screening. Unbeknownst to Hope and Prudence, identical forms of cancer develop in both twins at the exact moment in time, in 1990. Hope's tumor is detected by the screening test in 1990, and she undergoes surgical treatment and chemotherapy for five years. She dies in 2000. Her survival period after diagnosis is 10 years. Prudence, in contrast, is not screened with the test. She only detects her tumor when she feels a growing lump in her breast in 1999. She, too, has treatment, with some marginal benefit, and then relapses and dies at the same moment as Hope in 2000. Her survival time is one year. At the joint funeral, as the mourners stream by the identical caskets, an argument breaks out between Hope's and Prudence's doctors. Hope's physicians insist that she had a 10-year survival: her tumor was detected in 1990 and she died in 2000. Prudence's doctors insist that her survival was one year: her tumor was detected in 1999 and she died in 2000. Yet both cannot be right: the twins died from the same tumor at the exact moment in time. The solution to this seeming paradox, called "lead-time bias," is immediately obvious. Using survival as an endpoint for a screening test is flawed because early detection pushes the clock of diagnosis backwards. Hope's tumor and Prudence's tumor possess exactly identical biological behavior. But since doctors detected Hope's tumor earlier, it seems, falsely, that she lived longer and that the screening test was beneficial. There is a simple way to avoid this bias. Rather than measuring survival rates, one can measure the overall mortality. In other words, one can calculate exactly how many people died of cancer in 1970, versus 1990, versus 2010, and so forth, and plot this as a graph. But here too, there are methodological glitches. "Cancer-related death" is a raw number in a cancer registry, a statistic that arises from the diagnosis entered by a physician when pronouncing a patient dead. The problem with comparing that raw number over long stretches of time is that the American population (like any population) is itself gradually aging, and the rate of cancer-related mortality naturally increases as well. Old age inevitably drags cancer with it, like flotsam floating on a tide. A nation with a larger fraction of older citizens will seem more cancer-ridden than a nation with younger citizens, even if actual cancer mortality has not changed. To compare samples over time, some means is needed to normalize two populations to the same standard — in effect, by statistically "shrinking" one into another. The statistician John Bailar has performed exactly this form of analysis. He has normalized all populations from 1980 onwards, and measured cancer-specific death over time. And his analysis is accurate, but also sobering. Cancer-specific deaths are, in fact, trending downwards. They have been doing so for nearly a decade. But the downwards trend is not a steep slope towards zero. The figure below provides an even more sophisticated answer to this question: it divides cancer mortality by age groups and trends these over time. Once again, the answer is obvious. In men and women in the age groups 45-49 and 55-59, there has been a distinct downward trend (from 2 per 1000 to 1 per 1000 in men and women age 50-59). In contrast, for older men and women (75-79), the rates have risen, plateaued, and finally have begun to drop. Much of this rise is the result of the increase in lung cancer due to increased smoking in the 1960s. 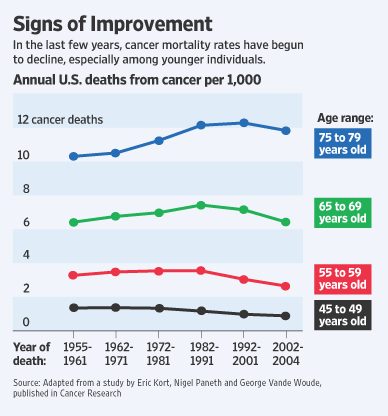 The epidemiologist Lester Breslow proposes yet another alternative metric to measure progress. If chemotherapy cures a five-year old child of leukemia, then it saves a full 65 years of potential life (given an overall life expectancy of about 70). In contrast, the chemotherapeutic cure in a 65-year-old man contributes only five additional years, given a life expectancy of 70. The metrics described above — age-adjusted mortality — cannot detect any difference in the two cases. A young woman cured of lymphoma, with 50 additional years of life, was judged by the same metric as an elderly woman cured of breast cancer, who might succumb to some other cause of death in the next year. In contrast, if "years of life saved" are used to judge progress, then the picture changes again: Breslow notes, "In 1980, cancer was responsible for 1.824 million lost years of potential life in the United States to age 65. If, however, the cancer mortality rates of 1950 had prevailed, 2.093 million years of potential life would have been lost." Whether you call this "progress" or "victory" is a personal decision. But measuring it turns out to be far more complex than we might have
|
Guests
by Siddhartha Mukherjee, November 17, 2010 9:43 AM
 In 2009, a Maryland woman in perfect health discovered a solid, matted lymph node under her left arm. It was biopsied and found to be a malignant melanoma. It had evidently metastasized from a primary tumor somewhere else in her body (melanomas grow from skin cells, and they don't grow directly in lymph nodes). When she underwent scans to appropriately stage her disease, metastatic masses were found everywhere: in lungs, liver, and abdomen. Yet surprisingly, the primary cancer — the origin of her diffuse disease — was never found. Cases such as hers are relatively rare in oncology. They are called "carcinomas of unknown primary" or CUP. And they usually present a particular thorny therapeutic problem. A major emerging theme in cancer medicine is that every tumor-type is treated differently. Breast, prostate, lung, and uterine cancer are attacked with vastly different regimens of chemicals, and they respond very differently. So how on earth do you treat a cancer of unknown primary? In this particular case, the woman's tumor cells bore a distinct biological mark indicating their origin in the skin, thereby classifying this as a melanoma. But although that identification brought clarity about the origin of the cancer, it still provided little solace. Metastatic melanoma is one of the few variants of cancer for which no drug or therapy has ever been found to extend survival. Many other forms of cancer have marched ahead in therapeutic terms, notably breast and prostate cancer, lymphomas, and leukemias. Metastatic melanoma, in contrast, seems like a cancer frozen in time. It is likely that the survival of a woman diagnosed in 1609 is no different from a woman diagnosed in 2009. For decades, oncologists treating metastatic melanoma had a hazy clue about a kind of drug that might work. For reasons mysterious and unknown, some men and women with this cancer experience spontaneous remissions of their melanomas. Their tumors, having grown aggressively, suddenly begin to shrink on their own. The most prominent theory behind these spontaneous remissions was that the immune system was attacking the cancer. And yet, attempts to activate the immune system using drugs had never succeeded in large scale clinical trials. To understand the mechanism of an immunological attack on cancer, one needs to understand how the immune system works. Immune cells are designed to identify and eliminate foreign elements from the body. They do so by identifying particular markers — called "antigens" — on the foreign cells and attacking these markers. But cancer, of course, grows out of one's own body. It is not "foreign," but a corrupted version of a normal cell. How, then, might the immune system recognize and eliminate a cancerous variant of a normal cell? Generations of cancer immunologists have tried to answer this question by trying to identify "antigens" that are unique to cancer cells. For some cancers that happen to be caused by viruses, viral antigens might be attacked by the immune system. For other cancers, the answer is more complex. Certain "antigens" in the human body are manufactured only during fetal development, or only in the sperm or testes. For reasons not fully understood, the immune system in adults can recognize these as "foreign." And cancer cells, for yet unknown reasons, begin to manufacture some of these fetal "antigens." But even so, the immune system does not recognize the fetal antigen on a cancer cell as foreign. To a cancer immunologist, this represents a paradox. Many cancers possess neo-antigens that should be recognized as foreign and thus rejected from the body. And yet, the immune systems seem to be somehow paralyzed in cancer patients so that they fail to reject these cells. In other words, the problem is not the "visibility" of a cancer cell, but rather the blindness of the immune system. In the 1990s, an immunologist named James Allison hypothesized that the immune system, like many bodily systems, also possesses molecular checks and balances — accelerators and brakes — to prevent inappropriate activation. We know the dire consequences of inappropriate activation: diseases such as rheumatoid arthritis, or multiple sclerosis, in which the immune system begins to attack one's own body. To prevent such gratuitous attacks, the immune system has evolved a sophisticated system of molecular brakes. Many different, independent molecular gates need to be opened in an immunological cell before that cell can be fully activated. The presence of multiple gates acts like a safety latch system, preventing early or inappropriate activation. Allison was particularly interested in one such gate, a molecule called CTLA4. In the 1990s, Allison and others had shown that blockading CTLA4 in animals could unleash the immune system, allowing these animals to begin rejecting tumors that had been growing in their bodies. In 2008, Allison and others thus launched an enormous study to determine if blockading CTLA4 might work in human cancers. Their obvious choice was melanoma — the tumor in which those tantalizing spontaneous remissions had been observed. The results, published in the New England Journal of Medicine, tell a tantalizing story. In a randomized double-blinded study, CTLA4 blockade indeed increases the survival of patients with metastatic melanoma. And more: as Allison reminded me last week, this is the only drug that has ever shown an increase in survival in this disease. The noteworthy feature of this result is that, in principle, any cancer can be treated by the activation of the immune system. Leukemias, lymphomas, breast cancer — anything that might elicit an immune response might be attacked by re-awakened immune cells. Cancer immunologists often refer the immune system as a "sleeping giant." In melanoma, at least, the giant is stirring
|
Guests
by Siddhartha Mukherjee, November 16, 2010 9:18 AM
 For my week-long blog for Powell's.com, I'll be attempting something novel. Every day, I will pick a single recent case from my files that highlights a major new discovery in cancer science or cancer medicine. As always, the names and dates will be scrambled to protect the identities of patients. And I will provide a link to the major medical or scientific study that lies behind the case. My goal here is to demonstrate how every case in medicine is a story in its own right — and how grand ideas are inevitably concealed within the homunculus of each story. ÷ ÷ ÷ Robert Bernard was a 77-year old advertising executive diagnosed with advancing leukemia who came to the clinic seeking advice. Bernard came from a large, voluble French-Canadian family — and much of that family, as it turned out, was also in the room with him. His wife, two sons, and a daughter had flown into New York from various parts of the planet. They were a tight-knit group, talking each other in an internal language that needed few words. The father, children, and even their mother resembled each other so distinctly that it seemed each was another incarnation of the other, displaced by a few decades. The Bernards were a unit, and they knew it. The family wanted to do everything possible — chemotherapy, bone marrow transplantation, experimental drugs — if possible, all three. Robert agreed, nodding enthusiastically. I told him that he had a slim chance of a sustained response, and a slimmer chance of cure. But they had already made their mind up. We drafted a plan, involving a visit to place a centralized catheter to infuse the chemotherapy. Robert would return in a week, and we'd start right away. I finished my note and was about to move to my next patient, when the nurse knocked on the door. "Robert wants to ask a question," she said. She ushered him in — this time, alone. The man who came through that door was quite unlike the man I had seen with his family. Alone, without the pressure to satisfy his children, and without the desire to perform, Robert was a transformed patient. He knew his leukemia was incurable, he said. He knew the risks and benefits of trying the more aggressive form of chemo and transplantation. But it was only alone, without his family, that he could admit the inadmissible: he had no desire to try aggressive therapies. He wanted palliative care and supportive medicines — drugs to keep his blood counts high, drugs to relieve pain. In private, he was, in effect, retracting the plan that we had made. He was not depressed; his mind was clear, his goals lucid. I agreed. In a sense, the push-pull quality of Bernard's story was emblematic. This drama, or a variant of it, is played out in the clinic every day. Some patients (or their families) push for therapies in the hopes for the slim chances of longer survival. Others pull back; they want palliative and supportive care. Even the words "push" and "pull" become loaded. Pushing implies a positive force, a desire to succeed, no matter the slimness of chance. Pulling implies an acceptance of the inevitable, a decision to embrace death. But does "pushing" ahead with therapies always mean longer survival? Last summer, an enormous trial on lung cancer patients turned this idea on its head. The trial set out to answer an ambitious question. Metastatic lung cancer is typically a lethal disease: with conventional chemotherapy, only 5% of patients survive at 5 years. So palliative care, rather than chemotherapy, is a perfectly reasonable option. The assumption was that palliative care might increase the quality of a patient's life, but might come at the cost of survival. But when the trial was completed, there was a surprise: palliative care did not merely alter quality of life, it actually increased survival. These results give us pause about how we think about "palliative care." As one of the leading researchers on the study put it: "One of the most common misconceptions about palliative care is that it indicates treatment has failed — that it means giving up. [But] in this study the addition of palliative care early in the course of illness extended the survival of patients with incurable lung cancer. These patients not only lived longer, but also experienced improved quality of life and were better able to enjoy the time they had remaining." In the case of metastatic lung cancer, at least, palliation was not just life-enhancing, but
|
Guests
by Siddhartha Mukherjee, November 15, 2010 10:07 AM
 For my week-long blog for Powell's, I'll be attempting something novel. Every day, I will pick a single recent case from my files that highlights a major new discovery in cancer science or cancer medicine. As always, the names and dates will be scrambled to protect the identities of patients. And I will provide a link to the major medical or scientific study that lies behind the case. My goal here is to demonstrate how every case in medicine is a story in its own right — and grand ideas are also concealed within each story. ÷ ÷ ÷ In the summer of 2009, a friend of mine awoke one night as if from a nightmare — flushed, hot, and short of breath, with a powerful fluttering in his chest. He thought he was having a heart attack. He was 43, an acclaimed writer about cities and urbanism, and in otherwise excellent health. That evening, he had made himself a particularly high-voltage version of the chili that he loved, spiced with the hottest Indian peppers in the world (in large part, our friendship is based on the mutual admiration of chili peppers). He went to see his doctor the next week, and was tested with an EKG, which was normal. "It's probably heartburn," she said, reassuringly. But then, almost as an afterthought, she thought she would scan his chest. And there it was in the scan: a spiculated, two-inch shadow in his chest that, biopsied, turned out to be the earliest stages of lung cancer. A few weeks later, a surgeon removed the mass, carefully excising it out of the lung with wide margins around. My friend has likely been cured — but by a strange confluence of luck and spices. Cases like his are fleetingly rare. Lung tumors are almost always only detected in advanced stages, and even with chemotherapy, surgery, and radiation, cure rates for advanced lung cancer have remained unchanged for decades. My friend's cancer was obviously detected by chance, but, in the spirit of a true gastronome, he attributes its detection to his beloved peppers. "Add yet another virtue to them," he said recently, "they literally saved my life." Lung cancer, oncologists know, is an inherently insidious disease. Locked away in the airy reticulations of the lung, most tumors become symptomatic only in late stages — often after they've transambulated to the bones, or the brain. And yet, caught in its earliest stages, lung cancer is curable. (The numbers tell the full story: patients with stage I lung cancer have a 75% survival at 5 years; patients with stage IV cancer have a 5% survival rate.) The stage-specificity of cure raises an important question: What if we could screen the entire asymptomatic population of men and women and thus catch lung cancer in its earliest stages? By the mid-1980s, several trials had shown that mammograms, which can detect early breast cancer, decreased the mortality from breast cancer. Extending that logic to lung cancer made obvious sense. Trial upon trial was thus launched to use X-rays to detect early lung cancer. But every trial was negative. For unknown reasons, the strategy that had worked in breast cancer — detecting early tumors using radiography — simply failed to work in lung cancer. Frustrated, researchers added an important variation to this study: rather than screening the population in general, they thought they would screen men and women at highest risk: long-term smokers. But even narrowing the focus to the highest risk group didn't succeed. The technology was too crude to work. Last month, at the end of nearly three decades of frustration, the National Cancer Institute announced a strikingly positive trial. In the so-called National Lung Screening Trial (NLST), more than 50,000 high risk smokers (men and women with more than 30 pack-years of smoking) were screened with CT scans. The first patients were randomized in 2002. The initial plan was to continue the study over nearly a decade. But the trial observers had to stop the trial before it was over. Clinical trials often get stopped for two reasons: either the drug or method being tested is found to be unexpectedly toxic, or the drug or method is found to be unexpectedly effective. In the NLST (fortunately) it was the latter. By late October 2010, 354 lung cancer deaths had occurred among those who had been screened with CT scan versus 442 deaths among those who were not screened by CT scanning — a 20% reduction in lung cancer mortality. Researchers could no longer justify continuing the trial. The CT-unscreened group would need to be screened as well. What do we do with this information? Should we all start queuing for CT scans in the hopes of detecting pre-symptomatic tumors (like my friend's)? Obviously not. This screening program was launched on a very high-risk group of smokers and cannot be legitimately used for nonsmokers. But generalizing such a screening plan nationwide even among smokers would carry formidable costs — overburdening an already overburdened health care system. Should smokers bear the costs of screening? Obviously not, again: we don't expect men and women with high blood pressure to pay for their coronary surgery. Insurance, by its very nature, works on the distribution of risk. But what if that risk is increased by a particular behavior — smoking, in this case — and the technology to reduce the risk turns out to be laborious, time-consuming, and expensive? In a sense, the NLST has pushed the once-moribund field of lung cancer screening into astonishingly thorny territory. Its moral is illuminating. In medicine, it might be worthwhile to be careful what one wishes for. If the wish comes true — in this case, by reducing mortality with CT scanning — the problems raised might be even more acute than the problems
|